Obesity as a Result of Metabolic Disease: Polycystic Ovarian Syndrome
A woman walks into your office with lower back pain, but in your examination you additionally note that she is obese, has acne, and perhaps excessive facial hair. If you are like most doctors, you will judge this patient and respect her less, blaming her condition on her behavior versus some other condition. “She is letting herself go,” you may think. We can be harsh and judgmental when assessing obese patients and categorize them differently. A study performed by Johns Hopkins revealed that it is common for physicians to have less respect for obese patients than they have for slender patients.
I had thus categorized a patient whom I had treated for years for recurrent back pain. She also suffered from obesity in spite of running five miles every day and restricting her diet. I remember giving her a hard time about her weight from our initial visit.
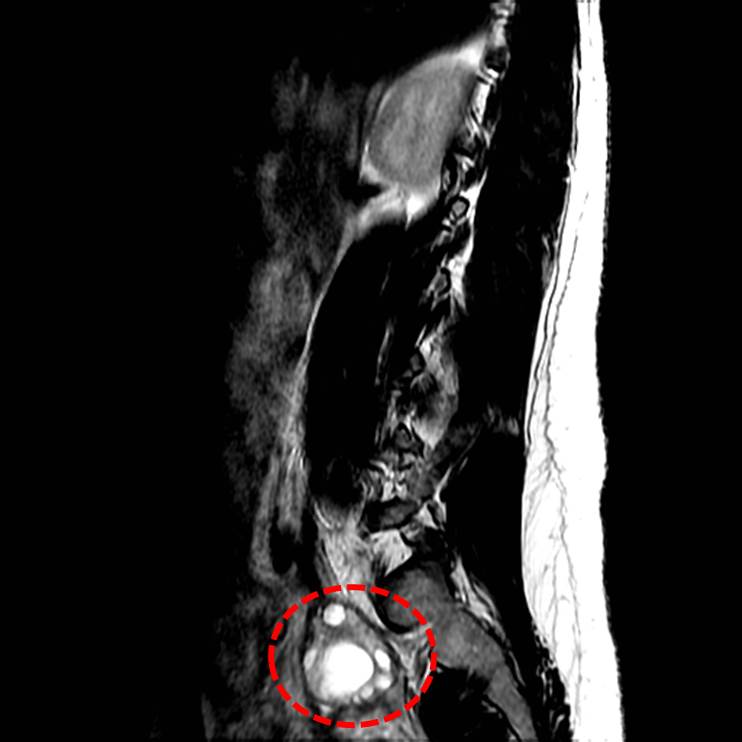
This went on for years until two things happened within a 24 hour period: First a colleague educated me about a condition known as Polycystic Ovarian Syndrome (PCOS), and then I noted on a lumbar MRI the coincidental presence of a polycystic ovary, a finding not mentioned in the MRI report. Then the lights went on in my mind. I identified my own personal prejudice about obesity and my patients who truly where heroically struggling to lose weight without effect.
What is Polycystic Ovarian Syndrome?
Polycystic Ovarian Syndrome gets its name from the characteristic enlarged ovaries with multiple small cysts around the outer edge of the ovary (or ovaries). The exact cause of PCOS is not known; in fact, I question whether the polycystic portion of the disease is a result of a more insidious underlying condition that results in ovarian disease and not the other way around.
PCOS results in the ovaries producing too much androgen (hormones associated with male characteristics). The symptoms commonly attributed to PCOS include obesity (though about 50% of the patients with PCOS are not obese), excessive facial and body hair, increased muscle size, reduced breast size, acne, and amenorrhea. Other effects include fertility issues, insulin resistance, type 2 diabetes, hypercholesterolemia, infrequent ovulation, and heart disease. Patients with PCOS are also at greater risk for hypertension, sleep apnea, and fatty liver disease. PCOS affects 5-10% of women in their childbearing years.
Diagnosis
The diagnosis of PCOS is difficult and probably should involve an interdisciplinary team. PCOS may be diagnosed by the presence of excessive androgen activity, infrequent ovulation, sporadic or absent menstrual cycles, and polycystic ovaries. Excessive androgen activity can be accessed clinically and in the lab through testing levels of androstenedione and testosterone. The ovaries can be visualized radiographically by diagnostic ultrasound and MRI.
Management
Since the presentation, diagnosis, and treatment for this malady is a bit nebulous, it is difficult to dictate a cut and dry management program. But here are some suggestions:
- Show compassion. PCOS patients have punished themselves enough already. We need to be in their corner supporting and uplifting them.
- Manage sugar. Since this disease is characterized by insulin resistance it is imperative that the patient learn to manage sugar cravings and to enhance healthy glucose metabolism. This can be done through exercise and eliminating refined sugars and enriched carbohydrates. Eating small meals more frequently will help control glucose levels. One study (albeit a small study by Wang et al., July 2007 issue of Fertility and Sterility) showed a benefit to taking ¼ to ½ teaspoon of cinnamon daily to help regulate insulin sensitivity in patients with PCOS.
- Exercise. Daily exercise is required.
- Prescribe an anti-inflammatory diet and lifestyle.
There is much more that could be said about this condition. If you are inexperienced in providing care of patients of this type I would recommend co-management with a physician with greater experience.
References
Wang JG, Anderson RA, Graham GM 3rd, Chu MC, Sauer MV, Guarnaccia MM, Lobo RA. The effect of cinnamon extract on insulin resistance parameters in polycystic ovary syndrome: a pilot study. Fertility Sterility. 2007 Jul;88(1):240-3.
Hoeger, KM. Obesity and Lifestyle Management in Polycystic Ovary Syndrome. Clinical Obstetrics and Gynecology. 2007; 50: 277-294.
Johns Hopkins News Release: